The coronavirus variant behind Brazil’s ferocious second wave of COVID-19 emerged, in part, because of relaxed social distancing, according to an analysis of viral sequences from the outbreak’s epicentre
Study examines measures to slow COVID-19 spread
Modeling of SARS-CoV-2 spread in Hunan, China showed that a minority of people infected with COVID-19 transmitted most infections. More than half of infections were spread before infected people developed symptoms. The findings could help inform better policies to control the spread of COVID-19 while balancing economic impact.
Link to article: https://www.nih.gov/news-events/nih-research-matters/study-examines-measures-slow-covid-19-spread
SARS-CoV-2 is transmitted predominantly through air
The coronavirus SARS-CoV-2 is transmitted predominantly through the air — by people talking and breathing out large droplets and small particles called aerosols. Catching the virus from surfaces — although plausible — seems to be rare. Despite this, some public-health agencies still emphasize that surfaces pose a threat and should be disinfected frequently. The result is a confusing public message.
Link to article: https://www.nature.com/articles/d41586-021-00277-8
Lessons learnt from easing COVID-19 restrictions: an analysis of countries and regions in Asia Pacific and Europe
Experts compare strategies for easing lockdown restrictions in Europe and Asia Pacific and identify key cross-country lessons – knowledge of infection levels, community engagement, public health capacity, health system capacity, and border control measures. They find an absence of clear and consistent strategies for exiting restrictions and identify key cross-country lessons that can still be learnt. Experience with past pandemics in Asia Pacific meant they were more prepared than European countries. An ambition to achieve a ‘Zero COVID’ strategy (eliminating domestic transmission), like in New Zealand, should be considered, suggest the authors.
Link to article https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(20)32007-9/fulltext
Spam Epidemiology and transmission dynamics of COVID-19 in two Indian states
A new study of more than a half-million people in India who were exposed to the novel coronavirus suggests that the virus’ continued spread is driven by only a small percentage of those who become infected, known as superspreaders. The study also found that children and young adults are potentially much more important to transmitting the virus than previously thought. The paper is the largest COVID-19 contact-tracing study to date.
Link to Study https://science.sciencemag.org/content/early/2020/09/29/science.abd7672.full
Social distancing to slow the US COVID-19 epidemic: Longitudinal pretest–posttest comparison group study
Across US States social distancing measures played a major role in slowing the spread of COVID-19 this spring, researchers have reported. Between March 10 and March 25, all 50 American states and the District of Columbia adopted at least one form of social distancing. These restrictions prevented 621,000 cases of COVID-19 across the United States within three weeks of being implemented, the researchers estimated. In addition, after a state enacted social distancing, its rate of deaths related to COVID-19 dropped, on average, after one week.
Link to article: https://journals.plos.org/plosmedicine/article?id=10.1371/journal.pmed.1003244
Coronavirus (COVID-19) related mortality rates and the effects of air pollution
Long-term exposure to air pollution may increase the risk of death from Covid-19, according to a large study. It analysed more than 46,000 coronavirus deaths in England and showed that a small, single-unit increase in people’s exposure to small-particle pollution over the previous decade may increase the death rate by up to 6%. A single-unit increase in nitrogen dioxide, which is at illegal levels in most urban areas, was linked to a 2% increase in death rates.
Structural basis of RNA cap modification by SARS-CoV-2
A new treatment idea for COVID-19 is possible after the discovery of the reason why the virus is so dangerous. The pathogen camouflages itself after infecting cells to prevent a swift response from the immune system. An enzyme the virus produces that tricks cells into believing the viral RNA belongs there has been identified. This mechanism delays the immune response and allows the virus to replicate inside cells. Therapies targeting the enzyme could prevent the pathogen from hiding in plain sight.
Link to article https://www.nature.com/articles/s41467-020-17496-8
Face masks including home-made ones contribute to reducing SARS-CoV-2 transmission
The Royal Society’s Face mask report says if correctly used face masks, including homemade cloth masks, can contribute to reducing viral transmission. Masks can offer an important tool for contributing to the management of community transmission of Covid19 within the general population. The report says evidence supporting their potential effectiveness comes from analysis of (1) the incidence of asymptomatic and pre-symptomatic transmission; (2) the role of respiratory droplets in transmission, which can travel as far as 1-2 meters; and (3) studies of the use of homemade and surgical masks to reduce droplet spread.
Link to report: https://rs-delve.github.io/reports/2020/05/04/face-masks-for-the-general-public.html
Peer review shows promising results of new vaccine against SARS CoV-2 virus
A paper in the New England Journal of Medicine reports on a trial of 45 healthy adults aged 18-55, each vaccinated twice, 28 days apart, with the mRNA-1273 vaccine developed by the National Institute of Allergy and Infectious Diseases (NIAID) and pharmaceutical company Moderna. All participants subsequently produced antibodies against the SARS CoV-2 virus, and their blood serum showed neutralizing activity against the virus, preventing it from entering cells. Moreover, the vaccine appears to provide stronger protection against new infections than an average bout of actually catching the disease.
Link to paper: https://www.nejm.org/doi/full/10.1056/NEJMoa2022483?query=featured_home
Longitudinal evaluation and decline of antibody responses in SARS-CoV-2 infection
Researchers say that antibodies in patients who have become infected by the virus may decline, or even disappear, within months, suggesting immunity from an eventual vaccine could fade as well over. Only 17% of the 60% of patients who had had a particularly strong antibody response when they were fighting the virus still had those antibodies at the same levels three months later. In some cases, the antibodies disappeared entirely, the researchers found. The study, if backed up by further evidence, would further undermine the concept of herd immunity.
Link to study: https://www.medrxiv.org/content/10.1101/2020.07.09.20148429v1
It is Time to Address Airborne Transmission of COVID-19
Converging lines of evidence indicate that SARS-CoV-2, the coronavirus responsible for the COVID-19 pandemic, can pass from person to person in tiny droplets called aerosols that waft through the air and accumulate over time. An international group of 237 clinicians, infectious-disease physicians, epidemiologists, engineers, and aerosol scientists have published a commentary in the journal Clinical Infectious Diseases that urges the medical community and public health authorities to acknowledge the potential for airborne transmission. They also call for preventive measures to reduce this type of risk.
Link to article https://academic.oup.com/cid/article/doi/10.1093/cid/ciaa939/5867798
Genomewide Association Study of Severe Covid-19 with Respiratory Failure
Study shows that people with Type A blood have a higher risk of catching coronavirus and of developing severe symptoms, while people with Type O blood have a lower risk. People with Type A blood had a 45% higher risk of becoming infected than people with other blood types, and people with Type O blood were just 65% as likely to become infected as people with other blood types.
Link to study: https://www.nejm.org/doi/full/10.1056/NEJMoa2020283
Coronavirus testing indicates transmission risk increases along wildlife supply chains for human consumption in Viet Nam
Study shows that field rats sold in markets and restaurants of Southeast Asia harbour multiple coronaviruses, a study shows. The proportion of positives increased as live animals were moved from “field to fork”, suggesting they were picking up viruses in the process. The strains detected are different from Covid-19 and are not thought to be dangerous to human health. However, scientists have warned that the wildlife trade is an incubator for disease. The mixing of multiple coronaviruses, and their amplification along the supply chain into restaurants, suggests “maximal risk for end consumers”.
Link to study: https://www.biorxiv.org/content/10.1101/2020.06.05.098590v1
Rationing social contact during the COVID-19 pandemic: Transmission risk and social benefits
The study identifies the businesses that have the best overall risk-benefit profiles when weighing important factors such as essential value to shoppers and the economy, as well as the relative risk of contracting COVID-19—or as one researcher put it, which businesses give us the most bang for our buck. At the top of the pile are banks, which are economically important yet uncrowded and visited infrequently.
Link to study: https://www.pnas.org/content/early/2020/06/09/2008025117
Prevalence of Asymptomatic SARS-CoV-2 Infection: A Narrative Review
Up to 45 percent of SARS-CoV-2 infections may be asymptomatic a new study shows. Asymptomatic infections may have played a significant role in the early and ongoing spread of COVID-19 and highlight the need for expansive testing and contact tracing to mitigate the pandemic.
Link to Study: https://www.acpjournals.org/doi/10.7326/M20-3012
Identifying airborne transmission as the dominant route for the spread of COVID-19
A comprehensive study shows wearing masks significantly reduces the number of infections, far more than other measures such as social distancing. It shows that airborne transmission is highly virulent and dominates the spread of COVID-19. It reveals that the difference with and without masks represents the determinant in shaping the trends of the pandemic.
Link to article: https://www.pnas.org/content/early/2020/06/10/2009637117
Governance, technology and citizen behavior in pandemic: Lessons from COVID-19 in East Asia
This paper analyzes the responses in East Asian countries and provides some commonalities and lessons. While countries have different governance mechanisms, it was found that a few governance decisions in respective countries made a difference, along with strong community solidarity and community behavior. Although the pandemic was a global one, its responses were local, depending on the local governance, socio-economic, and cultural context.
Link to article: https://www.sciencedirect.com/science/article/pii/S2590061720300272
The effect of travel restrictions on the spread of the 2019 novel coronavirus (COVID-19) outbreak
Paper published in Science looks at how travel and quarantine influence the dynamics of the spread of COVID-19. It concludes that the travel quarantine introduced in Wuhan on 23 January 2020 only delayed epidemic progression by 3 to 5 days within China, but international travel restrictions did help to slow spread elsewhere in the world until mid-February. The results suggest that early detection, hand washing, self-isolation, and household quarantine will likely be more effective than travel restrictions at mitigating this pandemic.
Link to paper: https://science.sciencemag.org/content/368/6489/395.full
The landscape of host genetic factors involved in infection to common viruses and SARS-CoV-2
This study looks at certain genetic variations in people that are associated with susceptibility to infection and the diverse clinical presentation of coronavirus disease (COVID-19) – including asymptomatic cases and severe forms of the disease in younger patients.
Link to study: https://www.medrxiv.org/content/10.1101/2020.05.01.20088054v1
Selection of viral variants during persistent infection of insectivorous bat cells with Coronavirus
New paper shows that when exposed to the MERS Coronavirus (CoV) bat cells adapt—not by producing inflammation-causing proteins but rather by maintaining a natural antiviral response. Simultaneously, the MERS virus also adapts to the bat host cells by very rapidly mutating one specific gene. Operating together, these adaptations result in the virus remaining long-term in the bat but being rendered harmless. Instead of killing bat cells as the virus does with human cells, the MERS coronavirus enters a long-term relationship with the host, maintained by the bat’s unique ‘super’ immune system. SARS-CoV-2 is thought to operate in the same way. The work suggests that stresses on bats—such as wet markets, other diseases, and possibly habitat loss—may have a role in coronavirus spilling over to other species.
Link to paper: https://www.nature.com/articles/s41598-020-64264-1
Effect of Alert Level 4 on Reff : review of international COVID-19 cases
This study mapped the coronavirus epidemic curve for 25 countries and modeled how the spread of the virus has changed in response to the various lockdown measures. It classifies each country’s public health response using New Zealand’s four alert system. Levels 1 and 2 represent relatively relaxed controls, whereas levels 3 and 4 are stricter. By mapping the change in the effective reproduction number (Reff, an indicator of the actual spread of the virus in the community) against response measures, the research shows countries that implemented level 3 and 4 restrictions sooner had greater success in pushing Reff to below 1.
Stopping Deforestation Can Prevent Pandemics – Scientific American
This article in Scientific American points out that three-quarters of the emerging pathogens that infect humans leaped from animals, many of the creatures in the forest habitats that we are slashing and burning to create land for crops, including biofuel plants, and for mining and housing. The more we clear, the more we come into contact with wildlife that carries microbes well suited to kill us—and the more we concentrate those animals in smaller areas where they can swap infectious microbes, raising the chances of novel strains.
Link to article: https://www.scientificamerican.com/article/stopping-deforestation-can-prevent-pandemics/
CIDRAP report COVID-19 to spread up to 2 years
The new coronavirus is likely to keep spreading for at least another 18 months to two years—until 60% to 70% of the population has been infected, says a new report. The primary focus of these scenarios is on the Northern Hemisphere, but similar patterns could occur in the Global South, as well. The lack of robust healthcare infrastructure and comorbidities such as other infections, malnutrition, and chronic respiratory disease in certain areas of the Global South could result in the pandemic being even more severe in those areas, as was noted during the 1918-19 pandemic.
Link to PDF:  CIDRAP report COVID-19 to spread up to 2 years
CIDRAP report COVID-19 to spread up to 2 years
Cleaning and Disinfectant Chemical Exposures and Temporal Associations with COVID-19 — National Poison Data System, United States, January 1, 2020–March 31, 2020
Calls to poison control centers in March surged by almost 20% compared to the same period in 2019, according to a new report released by the U.S. Centers for Disease Control and Prevention. Associated with the increased use of cleaners and disinfectants is the possibility of improper use, such as using more than directed on the label, mixing multiple chemical products together, not wearing protective gear, and applying in poorly ventilated areas.
Link to report: https://www.cdc.gov/mmwr/volumes/69/wr/mm6916e1.htm
Misinformation During a Pandemic leads to negative health outcomes
A novel study looking at impacts of coverage of COVID-19 by two Fox News shows in the United States – Hannity and Tucker Carlson Tonight – on viewers’ behavior and downstream health outcomes. Carlson warned viewers about the threat posed by the coronavirus from early February, while Hannity originally dismissed the risks associated with the virus before gradually adjusting his position starting late February. Hannity’s viewers changed behavior in response to the virus later than other Fox News viewers, while Carlson’s viewers changed behavior earlier. Greater viewership of Hannity relative to Tucker Carlson Tonight is strongly associated with a greater number of COVID-19 cases and deaths in the early stages of the pandemic. The researchers say that provision of misinformation in the early stages of a pandemic can have important consequences for how a disease ultimately affects the population.
Link to paper: https://papers.ssrn.com/sol3/papers.cfm?abstract_id=3580487
When Confronting a Pandemic, We Must Save Nature to Save Ourselves
This is a well-written statement entitled “When Confronting a Pandemic, We Must Save Nature to Save Ourselves” from the Centre for American Progress. The statement says COVID-19 outbreak has laid bare the need for a more proactive and integrated approach to fight infectious disease epidemics, which are becoming more common in many regions around the world. Specifically, we need to address the problem at its root: the destruction of nature. Nature is connected to human health, from the inherent mechanisms through which ecosystems regulate the emergence of new pathogens to the health benefits of spending time outdoors. But in our destruction of earth’s natural resources, we are losing these free services and reducing our resilience to new diseases.
Link to PDF:  When Confronting a Pandemic, We Must Save Nature to Save Ourselves
When Confronting a Pandemic, We Must Save Nature to Save Ourselves
Outcomes of hydroxychloroquine usage in United States veterans hospitalized with Covid-19
A pre-print of the results of a study of 386 coronavirus patients in a US government hospital for military veterans found more deaths among those treated with hydroxychloroquine than those treated with standard care. These findings highlight the importance of awaiting the results of ongoing prospective, randomized, controlled studies before widespread adoption of this drug, say the authors of the study.
Link to article: https://www.medrxiv.org/content/10.1101/2020.04.16.20065920v2
How they flattened the curve during the 1918 Spanish Flu
This is an article in National Geographic and not a scientific paper but it shows with graphs and a lot of references that social distancing isn’t a new idea and it saved thousands of American lives during the last great pandemic in 1918.
Link to article: https://www.nationalgeographic.com/history/2020/03/how-cities-flattened-curve-1918-spanish-flu-pandemic-coronavirus/
COVID-19: four-fifths of cases are asymptomatic, China figures indicate
New evidence has emerged from China indicating that the large majority of coronavirus infections do not result in symptoms. Experts say that it was quite likely that the virus had been circulating for longer than generally believed and that large swathes of the population had already been exposed.
Link to article: https://www.bmj.com/content/369/bmj.m1375
Phylogenetic network analysis of SARS-CoV-2 genomes
New important research shows early ‘evolutionary paths’ of COVID-19 in humans – as the infection spread from Wuhan out to Europe and North America – using genetic network techniques. The research revealed three distinct ‘variants’ of COVID-19, consisting of clusters of closely related lineages, which they label ‘A’, ‘B’ and ‘C’. Variant ‘A’, most closely related to the virus found in both bats and pangolins, is described as ‘the root of the outbreak’. Type ‘B’ is derived from ‘A’, separated by two mutations, then ‘C’ is in turn a “daughter” of ‘B’.
Link to article: https://www.pnas.org/content/early/2020/04/07/2004999117
Model quantifies the impact of quarantine measures on Covid-19’s spread
MIT has developed a model to determine the efficacy of quarantine measures and better predict the spread of the virus. The model found that in places where strong measures were implemented quickly, the quarantine effort could effectively curb the spread of the virus. In places where the quarantine efforts were rolled out slowly, the effort to slow the spread has been less effective. The model predicts when the coronavirus ‘plateau’ will take place, finding that the cases aren’t likely to start stagnating until some time between April 15 and April 20. It says that restrictions on quarantine can only be made when multiple conditions are met, including when the transmission is controlled, hospitals have capacities to meet all the needs of the public, workplaces have effective preventative measures in place, and more.
Link to article: http://news.mit.edu/2020/new-model-quantifies-impact-quarantine-measures-covid-19-spread-0416
Sub-Saharan Africa Regional Economic Outlook
The International Monetary Fund (IMF) has released its Economic Outlook for Sub-Saharan Africa. The health crisis has precipitated an economic crisis reflecting three large shocks: disruption of production and a sharp reduction in demand; spillovers from a sharp deterioration in global growth and tighter financial conditions; and a severe decline in commodity prices. As a result, the region’s economy is projected to contract by 1.6 percent this year—the worst-reading on record. Some economies such as this highly dependent on tourism are expected to shrink further.
Link to publication: https://www.imf.org/en/Publications/REO/SSA/Issues/2020/04/01/sreo0420
Determining the optimal duration of the COVID- 19 suppression policy: A cost-benefit analysis
The paper published on March 27 by the American Enterprise Institute compared the economic costs of businesses staying closed, which causes a steep drop in the gross domestic product, with the economic benefits of a lockdown. The research found that for at least two more months, the economic benefits of controlling the virus and preventing illness and death are greater than the economic cost of closing most non-essential businesses. It also found that even after the lockdown is lifted, we must keep in place more moderate measures, such as wearing face masks and limiting public gatherings, until a vaccine or an effective drug or treatment becomes widely available.
Extreme genomic CpG deficiency in SARS-CoV-2 and evasion of host antiviral defense
New genetic analysis of SARS-CoV-2 and related coronaviruses suggests the ancestor of COVID-19 and its nearest relative — a bat coronavirus — infected the intestine of dogs, most likely resulting in a rapid evolution of the virus and its jump into humans. This suggests the importance of monitoring SARS-like coronaviruses in feral dogs. It is to be noted however that other experts have doubts.
Link to article: https://academic.oup.com/mbe/article/doi/10.1093/molbev/msaa094/5819559
Projecting the transmission dynamics of SARS-CoV-2 through the postpandemic period
The paper projects that the US may have to endure social distancing measures — such as stay-at-home orders and school closures — until 2022, unless critical care capacity is increased substantially or treatment or vaccine becomes available. Another round of the virus is possible once social distancing measures are lifted. Even in the event of apparent elimination, SARS-CoV-2 surveillance should be maintained since a resurgence in contagion could be possible as late as 2024.
Link to paper: https://science.sciencemag.org/content/early/2020/04/14/science.abb5793.full
Global shifts in mammalian population trends reveal key predictors of virus spillover risk
Paper shows that wild mammals that were at risk of extinction owing to human activities carried twice the zoonotic diseases compared to animals that were not at the same risk. Among threatened wildlife species, those with population reductions owing to exploitation and loss of habitat shared more viruses with humans. This has increased opportunities for animal-human interactions and facilitated zoonotic-disease transmission.
Link to article: https://royalsocietypublishing.org/doi/10.1098/rspb.2019.2736
Mortality associated with COVID-19 outbreaks in care homes: early international evidence
About half of all Covid-19 deaths appear to be happening in care homes in some European countries, according to early figures. Snapshot data from varying official sources shows that in Italy, Spain, France, Ireland and Belgium between 42% and 57% of deaths from the virus have been happening in care homes (non-acute residential and nursing facilities that house people with some form of long-term care needs).
Link to PDF:  Mortality associated with COVID-19 outbreaks in care homes: early international evidence
Mortality associated with COVID-19 outbreaks in care homes: early international evidence
Wet markets—a continuing source of severe acute respiratory syndrome and influenza?
A paper published in 2004 warning that wet markets provide optimum conditions for amplification and perpetration of disease agents such as influenza and the evolution of infectious disease agents.
Link to article: https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(03)15329-9/fulltext
Effect of non-pharmaceutical interventions for containing the COVID-19 outbreak in China
Study shows that by the end of February 2020 without non-pharmaceutical interventions (NPIs) in China– such as early detection, isolation of cases and social distancing – the number of infected people would have been 67 times larger than that which occurred. If NPIs could have been conducted one week, two weeks, or three weeks earlier in China, cases could have been reduced by 66%, 86%, and 95%, respectively, together with significantly reducing the number of affected areas. Improved disease detection, isolation of cases and social distancing are likely to a far greater positive impact on containment than travel restrictions, says the study.
Link to study: https://www.medrxiv.org/content/10.1101/2020.03.03.20029843v3
Considerations for Drug Interactions on QTc in Exploratory COVID-19 (Coronavirus Disease 2019) Treatment
In a joint statement on April 8, the American Heart Association, the American College of Cardiology, and the Heart Rhythm Society cast doubts as to the safety of hydroxychloroquine and azithromycin for potential prophylaxis or treatment for COVID-19; both drugs are listed as definite causes of torsade de pointes” and increase in the risk of other arrhythmias and sudden death”, the statement says. In addition “seriously ill patients often have comorbidities that can increase risk of serious arrhythmias,” including hypokalemia, hypomagnesemia, fever, and systemic inflammation, the groups said.
Link to PDF:
 Considerations for Drug Interactions on QTc in Exploratory COVID-19 (Coronavirus Disease 2019) Treatment
Considerations for Drug Interactions on QTc in Exploratory COVID-19 (Coronavirus Disease 2019) Treatment
How does COVID-19 kill? Uncertainty is hampering doctors’ ability to choose treatments
How does COVID-19 kill? Uncertainty over whether it is the virus itself — or the response by a person’s immune system — that ultimately overwhelms a patient’s organs, is making it difficult for doctors to determine the best way to treat patients who are critically ill with the coronavirus. Clinical data suggest that the immune system plays a part in the decline and death of people infected with the new coronavirus, and this has spurred a push for treatments such as steroids that rein in that immune response. But some of these treatments act broadly to suppress the immune system.
Link to article: https://www.nature.com/articles/d41586-020-01056-7
Effectiveness of convalescent plasma therapy in severe COVID-19 patients
A new preliminary study shows a single 200 mL dose of convalescent plasma (CP) from COVID-19 patients who recently recovered shortened the duration of symptoms, improved oxygen levels and increased the clearance of the virus in patients who were still suffering from the disease. “One dose of convalescent plasma with a high concentration of neutralizing antibodies can rapidly reduce the viral load and tends to improve clinical outcomes”.
Habitat fragmentation, livelihood behaviors, and contact between people and nonhuman primates in Africa
A new paper shows that the destruction of forests into fragmented patches is increasing the likelihood that viruses and other pathogens will jump from wild animals to humans.
Link to paper: https://link.springer.com/article/10.1007/s10980-020-00995-w
Potential vulnerability of COVID-19
An antibody recovered from a survivor of the SARS epidemic in the early 2000s has revealed a potential vulnerability of the new coronavirus at the root of COVID-19.
Published in Science, the study is the first to map a human antibody’s interaction with the new coronavirus at near-atomic-scale resolution. Although the antibody was produced in response to an infection of SARS, which is caused by the SARS-CoV virus, it cross-reacts with the new coronavirus, SARS-CoV-2.
Link to study: https://science.sciencemag.org/content/early/2020/04/02/science.abb7269.full
The FDA-approved Drug Ivermectin inhibits the replication of SARS-CoV-2 in vitro
Study showed that a single dose of the drug, Ivermectin, could stop the SARS-CoV-2 virus growing in cell culture – effectively eradicating all genetic material of the virus within 48 hours. Ivermectin is an anti-parasitic drug that has also been shown to be effective in vitro against a broad range of viruses including HIV, Dengue, Influenza and Zika virus.
Link to study: https://www.sciencedirect.com/science/article/pii/S0166354220302011
Coronavirus can infect cats — dogs, not so much
Cats can be infected with COVID-19 and can spread it to other cats, but dogs are not really susceptible to the infection, say researchers in China. The team, at Harbin Veterinary Research Institute, also concludes that chickens, pigs, and ducks are not likely to catch the virus. Other scientists say the findings are interesting but note the results are based on lab experiments in which a small number of animals were deliberately given high doses of the virus, SARS-CoV-2, and do not represent real-life interactions between people and their pets.
Link to article: https://www.nature.com/articles/d41586-020-00984-8
Correlation between universal BCG vaccination policy and reduced morbidity and mortality for COVID-19: an epidemiological study
A preprint of a study says that countries with mandatory policies to vaccinate against tuberculosis register fewer coronavirus deaths than countries that don’t have those policies.
Assessment of Narratives and Disinformation Around the COVID-19 Pandemic – EU vs DISINFORMATION
Disinformation and misinformation around COVID-19 continue to proliferate around the world, with potentially harmful consequences for public health and effective crisis communication. In the EU and elsewhere, coordinated disinformation messaging seeks to frame vulnerable minorities as the cause of the pandemic and to fuel distrust in the ability of democratic institutions to deliver effective responses.
Link to article: https://euvsdisinfo.eu/eeas-special-report-update-short-assessment-of-narratives-and-disinformation-around-the-covid-19-pandemic/
Rational use of face masks in the COVID-19 pandemic
Comparison of face mask use recommendations by different health authorities. Despite the consistency in the recommendation that symptomatic individuals and those in health-care settings should use face masks, differences in recommendations were observed for the general public and community settings. Evidence that face masks can provide effective protection against respiratory infections in the community is scarce. However, face masks are widely used by medical workers as part of droplet precautions when caring for patients with respiratory infections. The study suggests vulnerable individuals avoid crowded areas and use surgical face masks rationally when exposed to high-risk areas.
Link to article: https://www.thelancet.com/journals/lanres/article/PIIS2213-2600(20)30134-X/fulltext
Social distancing strategies for curbing the COVID-19 epidemic | medRxiv
In this pre-print a team from Harvard using mathematical model found that one-time interventions will be insufficient to maintain COVID-19 prevalence within the critical care capacity of the United States. Seasonal variation in transmission will facilitate epidemic control during the summer months but could lead to an intense resurgence in the autumn. Intermittent distancing measures can maintain control of the epidemic, but without other interventions, these measures may be necessary into 2022.
Link to article: https://www.medrxiv.org/content/10.1101/2020.03.22.20041079v1
Meteorological factors and Covid-19 incidence in 310 regions across the world
This study analyzed l data from 311 regions across 116 countries with reported cases of COVID-19 by March 12, 2020, and found that temperature, humidity, and wind speed were inversely associated with the incidence rate of Covid-19. This means that it is likely that as temperature, humidity and wind speed increase the spread of COVID-19 decreases.
Link to article: https://www.medrxiv.org/content/10.1101/2020.03.27.20045658v1
Mobility traces and spreading of COVID-19
The authors have built human mobility models, for which they are experts, and attach a virus infection dynamics to it. This results in a virus spreading dynamics model. The preliminary model shows that complete lockdown works. About 10 days after lockdown, the infection dynamics die down in the model. Infections in public transport play an important role, they say. The simulations say that complete removal of infections at child care, primary schools, workplaces and during leisure activities will not be enough to sufficiently slow down the infection dynamics.
Link to article: https://www.medrxiv.org/content/10.1101/2020.03.27.20045302v1
A mathematical model of COVID-19 transmission between frontliners and the general public | medRxiv
This study formulates a conceptual mathematical model on the transmission dynamics of COVID-19 between the frontliners (e.g. healthcare workers, customer service and retail personnel, food service crews) and the general public. The take-home message of this preliminary model is that everyone in the community, whether a frontliner or not, should be protected or should implement preventive measures to avoid being infected.
Link to article: https://www.medrxiv.org/content/10.1101/2020.03.27.20045195v1
Role of Chloroquine and Hydroxychloroquine in the Treatment of COVID-19 Infection- A Systematic Literature Review | medRxiv
This is a systematic literature review summarizing the available evidence regarding the role of chloroquine in treating coronavirus infection. It says there is theoretical, experimental, preclinical and clinical evidence of the effectiveness of chloroquine in patients affected with COVID-19. There is adequate evidence of drug safety from the long-time clinical use of chloroquine and hydroxychloroquine in other indications. More data from ongoing and future trials will add more insight into the role of chloroquine and hydroxychloroquine in COVID-19 infection it concludes.
Link to article: https://www.medrxiv.org/content/10.1101/2020.03.24.20042366v1
Association of Cardiac Injury With Mortality in Hospitalized Patients With COVID-19 in Wuhan, China
New study in JAMA Cardiology says COVID-19 can not only be deadly for people with existing heart conditions, but it can also cause cardiac injury for people without pre-existing heart conditions. The study looked at 416 COVID-19 patients hospitalized in Wuhan, China and found that 19.7% suffered a cardiac injury, which put them at higher risk for a fatal version of Coronavirus.
Link to article: https://jamanetwork.com/journals/jamacardiology/fullarticle/2763524
Genetic variants of COVID-19
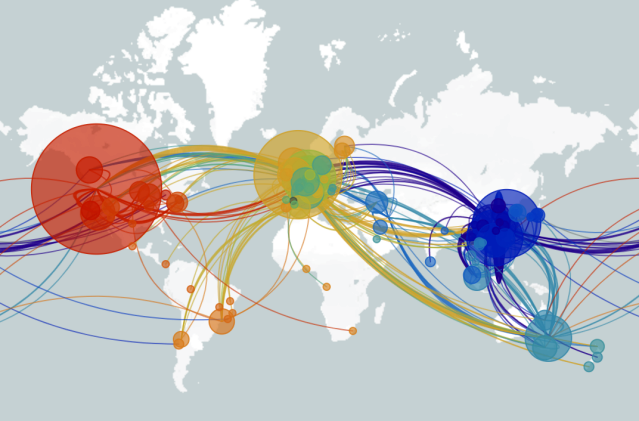
There are several genetic strains of COVID-19 circulating around the world. Information is found on NextStrain, an online resource for scientists that uses data from academic, independent and government laboratories all over the world to visually track the genomics of the SARS-CoV-2 virus. It currently represents genetic sequences of strains from 36 countries on six continents.
Link to article: https://nextstrain.org
A map of the main known genetic variants of the SARS-CoV-2 virus that causes COVID-19 disease. The map is being kept on the nextstrain.org website, which tracks pathogen evolution.
Physical interventions to interrupt or reduce the spread of respiratory viruses: systematic review
A wide-ranging study points out that simple public health measures seem to be highly effective at reducing the transmission of respiratory viruses. It recommends implementing the following interventions: frequent handwashing (with or without antiseptics), barrier measures (gloves, gowns, and masks), and isolation of people with suspected respiratory tract infections.
Link to article: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2190272/
What is the evidence for loss of smell and loss of taste as a clinical feature of COVID-19?
The authors are of the opinion that evidence regarding the complete loss of smell, or anosmia and the loss of taste or dysgeusia in people who had no other symptoms but who tested positive for COVID-19 are mostly anecdotal and therefore should be treated as preliminary and with caution.
Link to article: https://www.cebm.net/covid-19/what-is-the-evidence-for-anosmia-loss-of-smell-as-a-clinical-feature-of-covid-19/
Loss of sense of smell as marker of COVID.pdf
A Statement from ENT UK at The Royal College of Surgeons of England, the association of ear, nose and throat physicians in the United Kingdom says a growing body of data from COVID-19 patients in several countries strongly suggests that “significant numbers” of those patients experienced the complete loss of smell known as anosmia as one of the disease’s symptoms.
Link to PDF:  Loss of sense of smell as marker of COVID.pdf
Loss of sense of smell as marker of COVID.pdf
Covid 19 information for workplaces
We wish to share materials of relevance to workplaces that may help with:
· General education of all staff (general education – Covid 19.pdf) to better prepare themselves to take the required precautions and adopt safe behaviours.
Link to PDF:  general education – Covid 19.pdf
general education – Covid 19.pdf
· Guidance for workplaces on how best to prepare for Covid 19 ( Covid 19 advice for workplaces 3.0.pdf ).
Link to PDF:  Covid 19 advice for workplaces 3.0.pdf
Covid 19 advice for workplaces 3.0.pdf
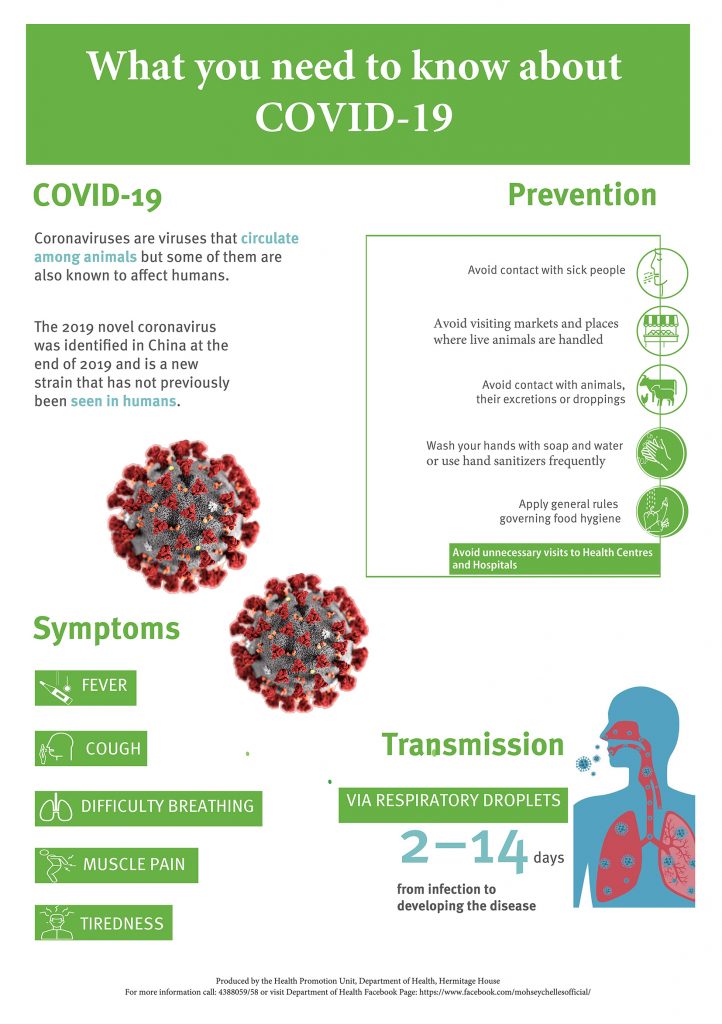
· Two local posters on Covid 19.

Identifying SARS-CoV-2 related coronaviruses in Malayan pangolins
A new paper, 26 March, describes multiple lineages of pangolin coronavirus and their similarity to the SARS-CoV-2. A previous study had suggested that Pangolins could be intermediate hosts. Although bats are likely reservoir hosts for SARS-CoV-2, this study says that pangolins should be considered as possible hosts in the emergence of novel coronaviruses and should be removed from wet markets to prevent zoonotic transmission. The study was done on Malayan pangolins (Manis javanica) seized in anti-smuggling operations in southern China. Pangolins are the world’s most trafficked animals.
Link to article: https://www.nature.com/articles/s41586-020-2169-0
Q&A: COVID-19 pandemic – impact on food and agriculture
The Food and Agriculture Organization (FAO) of the United Nations answers questions regarding the impact of the pandemic on food security
Link to article: http://www.fao.org/2019-ncov/q-and-a/en/
Can you boost your immune system against the coronavirus (COVID-19)?
The Australian Government’s Health Direct provides information on how to boost your immune system – it warns that currently there is no evidence that supplements are effective against COVID-19.
Link to article: https://www.healthdirect.gov.au/blog/can-you-boost-your-immune-system-against-the-coronavirus-covid-19
The SARS, MERS and novel coronavirus (COVID-19) epidemics, the newest and biggest global health threats: what lessons have we learned?
This paper finds that Inadequate risk assessment regarding the urgency of the situation, and limited reporting on the virus within China has, in part, led to the rapid spread of COVID-19. Compared with SARS and MERS, COVID-19 has spread more rapidly, due in part to increased globalization and the focus of the epidemic. The conclusion is that we did not learn from the two prior epidemics of coronavirus and were ill-prepared to deal with the challenges the COVID-19 epidemic has posed. Future research should attempt to address the uses and implications of the internet of things (IoT) technologies for mapping the spread of infection.
Link to paper: https://www.ncbi.nlm.nih.gov/pubmed/32086938
Expert comments about herd immunity
What is “herd immunity” and can we reach it for the current pandemic?
Link to article: https://www.sciencemediacentre.org/expert-comments-about-herd-immunity/
Expert reaction to schools being asked to close from Friday afternoon
Several experts talk about the closing of schools to combat the spread of COVID-19 in England.
Link to article: https://www.sciencemediacentre.org/expert-reaction-to-schools-being-asked-to-close-from-friday-afternoon/
Expert comment about COVID-19 and having sex while either socially distancing or self-isolating with symptoms
Prof Paul Hunter, Professor in Medicine, University of East Anglia, U.K, talks to the Science Media Centre on whether its advisable expert to have sex while either socially distancing or self-isolating with symptoms.
Link to article: https://www.sciencemediacentre.org/expert-comment-about-covid-19-and-having-sex-while-either-socially-distancing-or-self-isolating-with-symptoms/
Expert comment on age, COVID-19 infection and the role of social distancing
The Science Media Centre asks experts why it is important for young people to practice social distancing.
Link to article: https://www.sciencemediacentre.org/expert-comment-on-age-covid-19-infection-and-the-role-of-social-distancing/
We shouldn’t worry when a virus mutates during disease outbreaks
Mutation. The word naturally conjures fears of unexpected and freakish changes. Ill-informed discussions of mutations thrive during virus outbreaks, including the ongoing spread of SARS-CoV-2. In reality, mutations are a natural part of the virus life cycle and rarely impact outbreaks dramatically say virologists writing in the journal Nature Microbiology.
Link to article: https://www.nature.com/articles/s41564-020-0690-4
Are viruses alive?
Viruses are kind of mysterious – there is debate on whether on not they are “alive”. At a basic level, viruses are proteins and genetic material that survive and replicate within their environment, inside another life form. In the absence of their host, viruses are unable to replicate and many are unable to survive for long outside the host. Therefore, if they cannot survive independently, can they be defined as being ‘alive’? Taking opposing views, two microbiologists discuss how viruses fit with the concept of being ‘alive’ and how they should be defined.
Link to article: https://microbiologysociety.org/publication/past-issues/what-is-life/article/are-viruses-alive-what-is-life.html
WHO launches global megatrial of the four most promising coronavirus treatments
An article from the publishers of Science on 22 March on WHO megatrials. WHO is focusing on what it says are the four most promising therapies: an experimental antiviral compound called remdesivir; the malaria medications chloroquine and hydroxychloroquine; a combination of two HIV drugs, lopinavir, and ritonavir; and that same combination plus interferon-beta, an immune system messenger that can help cripple viruses.
Link to article: https://www.sciencemag.org/news/2020/03/who-launches-global-megatrial-four-most-promising-coronavirus-treatments
Twitter thread on Chloroquine (CQ) and Hydroxychloroquine (HCQ) by Dr. Gaetan Burgio
Unusually, we include a Twitter feed here as it represents a good analysis of the efficacy of the antimalarial drug chloroquine as a treatment for COVID-19. It is from Dr. Gaetan Burgio, a geneticist at the Australian National University who dug into the available & published data and reveals that as of this date the evidence remains anecdotal and a clinical trial is incomplete and not following scientific rigour. More research is needed.
Link to Twitter thread: https://twitter.com/GaetanBurgio/status/1241201751916568576
How blood from coronavirus survivors might save lives
A popular article from the publishers of Nature describing ongoing research that hopes that the antibody-laden blood of those who have recovered from coronavirus might reduce severe infections. It is as yet unknown if it will work.
Link to article: https://www.nature.com/articles/d41586-020-00895-8
Risk factors for human disease emergence.
Review identifies 1415 species of infectious organism known to be pathogenic to humans. Out of these, 868 (61%) are zoonotic, that is, they can be transmitted between humans and animals, and 175 pathogenic species are associated with diseases considered to be ’emerging’. Out of the emerging pathogens, 132 (75%) are zoonotic.
Link to article: https://www.ncbi.nlm.nih.gov/pubmed/11516376
Are hydroxychloroquine and azithromycin an effective treatment for COVID-19?
A discussion of whether hydroxychloroquine and azithromycin are an effective treatment for COVID-19 based on the latest research and knowledge.
Link to article: https://sciencebasedmedicine.org/are-hydroxychloroquine-and-azithromycin-an-effective-treatment-for-covid-19/
Clinical trials for hydroxychloroquine
At least six clinical trials for hydroxychloroquine are recruiting patients or in planning stages around the world.
Link to Search: https://clinicaltrials.gov/ct2/results?cond=COvid-19&term=hydroxychloroquine&cntry=&state=&city=&dist
NIH clinical trial of investigational vaccine for COVID-19 begins
March 17, 2020. A clinical trial of investigational vaccine for COVID-19 has begun. Phase 1 clinical trial evaluating an investigational vaccine designed to protect against coronavirus disease 2019 (COVID-19) has begun at Kaiser Permanente Washington Health Research Institute (KPWHRI) in Seattle. Currently (March 17, 2020) no approved vaccines exist to prevent infection with SARS-CoV-2.
Link to article: https://www.nih.gov/news-events/news-releases/nih-clinical-trial-investigational-vaccine-covid-19-begins
Severe Outcomes Among Patients with Coronavirus Disease 2019 (COVID-19) — United States, February 12–March 16, 2020
CDC Report: More than 40 percent of those who have tested positive for the virus in New York City are between the ages of 18 and 44.
Link to article: https://www.cdc.gov/mmwr/volumes/69/wr/mm6912e2.htm
How to stop future pandemics in 3 easy steps
While many of us are social distancing and self-quarantining, we have a lot of time to wonder, how did we get in this coronavirus mess in the first place? The answer is a zoonotic disease – a disease that can leap from animal to human. In order to prevent future pandemics, we need to change our relationship with wildlife. So what does that mean exactly?
1. Stop wildlife trade
2. Stop wildlife consumption
3. Stop destroying nature
Link to article: https://www.treehugger.com/health/how-stop-pandemics-3-steps.html
Public Health Responses to COVID-19 Outbreaks on Cruise Ships — Worldwide, February–March 2020
More than 800 cases of laboratory-confirmed COVID-19 cases occurred during outbreaks on three cruise ship voyages, and cases linked to several additional cruises have been reported across the United States. Transmission occurred across multiple voyages from ship to ship by crew members; both crew members and passengers were affected; 10 deaths associated with cruise ships have been reported to date.
Link to article: https://www.cdc.gov/mmwr/volumes/69/wr/mm6912e3.htm
Relationship between the ABO Blood Group and the COVID-19 Susceptibility
A new study shows people with blood group A have a significantly higher risk for acquiring COVID-19 whereas blood group O has a significantly lower risk for the infection. However, the paper has not been peer-reviewed yet. This means it has yet to be evaluated and so should not be used to guide clinical practice or to promote the results.
Link to article: https://www.medrxiv.org/content/10.1101/2020.03.11.20031096v1
Questions and Answers on the 2019 Coronavirus Disease (COVID-19 and pets
The World Organisation for Animal Health says that there have not been any reports of pets presenting clinical signs caused by COVID-19 virus infection and currently there is no evidence that they play a significant epidemiological role in this disease.
Linke to article: https://www.oie.int/en/scientific-expertise/specific-information-and-recommendations/questions-and-answers-on-2019novel-coronavirus/
Can Asia’s infectious disease-producing wildlife trade be stopped?
An article from the Food and Environment Reporting Network on Asia’s huge infectious disease-producing wildlife trade and whether it can be stopped.
Link to article: https://thefern.org/2020/03/can-asias-infectious-disease-producing-wildlife-trade-be-stopped/
Pangolins Decline as Deadly Poaching Continues, Red List Experts Find
All Asian Pangolin species, the worlds most traded wild animals, are Critically Endangered because of illegal trade. Now the species which may be the intermediate host of COVID-19 is in even more danger as panic killing may wipe them out.
Link to article: https://biologicaldiversity.org/w/news/press-releases/pangolins-decline-deadly-poaching-continues-red-list-experts-find-2019-12-10/
Mystery deepens over animal source of coronavirus
Scientists are racing to identify the source of the coronavirus and several papers have been published purporting bats to be the primary host and pangolins to be the intermediate carrier.
Link to article: https://www.nature.com/articles/d41586-020-00548-w
COVID-19: nitrogen dioxide over China
The pandemic is shutting down industrial activity and temporarily slashing air pollution levels over China, satellite imagery from the European Space Agency shows.
Linkt to data: https://www.esa.int/Applications/Observing_the_Earth/Copernicus/Sentinel-5P/COVID-19_nitrogen_dioxide_over_China
ACE inhibitors and angiotensin receptor blockers may increase the risk of severe COVID-19, paper suggests
This research proposes a possible explanation for the severe lung complications being seen in older people diagnosed with COVID-19 and also why young children seem protected against the disease.
Link to text: https://www.sciencedaily.com/releases/2020/03/200323101354.htm
A SARS-CoV-2-Human Protein-Protein Interaction Map Reveals Drug Targets and Potential Drug-Repurposing
Nearly 70 drugs and experimental compounds may be effective in treating the coronavirus, a team of researchers reported. To come up with the list, hundreds of researchers embarked on an unusual study of the genes of the coronavirus, also called SARS-CoV-2.
Link to article: https://www.biorxiv.org/content/10.1101/2020.03.22.002386v1
18 – Pandemics: Health Care Emergencies
This book chapter reviews the available mental health literature concerning the most impactful global infectious disease outbreaks. Case examples are used to illustrate mental health consequences. An overview of public health response and management of pandemic is reviewed throughout various disaster phases, and focused issues regarding mental health intervention planning for pandemics are discussed.
Link to review: https://www.cambridge.org/core/books/textbook-of-disaster-psychiatry/pandemics-health-care-emergencies/478824C480288A8935798FBF151D96FA
Mental Health and Faith Community Partnership
This article describes the Mental Health and Faith Community Partnership which is a collaboration between psychiatrists and clergy. The partnership provides an opportunity for psychiatrists and the mental health community to learn from spiritual leaders, to whom people often turn in times of mental distress. At the same time, it provides an opportunity to improve understanding of the best science and evidence-based treatment for psychiatric illnesses among faith leaders and those in the faith community.
Linke to article: https://www.psychiatry.org/psychiatrists/cultural-competency/engagement-opportunities/mental-health-and-faith-community-partnership
The H1N1 Crisis: A Case Study of the Integration of Mental and Behavioral Health in Public Health Crises
This paper looks at the H1N1 Crisis as a Case Study for the Integration of Mental and Behavioral Health in the epidemics of this kind.
Managing Anxiety & Stress
The outbreak of COVID-19 may be stressful for people. Fear and anxiety about a disease can be overwhelming and cause strong emotions in adults and children. This CDC guide provides advice on how to cope with the stress and make you, the people you care about, and your community stronger.
Linke to Guide: https://www.cdc.gov/coronavirus/2019-ncov/prepare/managing-stress-anxiety.html
The psychological impact of quarantine and how to reduce it: rapid review of the evidence
Decisions on how to apply quarantine should be based on the best available evidence. This paper reviews the psychological impact of quarantine using three electronic databases. Results show that in situations where quarantine is deemed necessary, officials should quarantine individuals for no longer than required, provide a clear rationale for quarantine and information about protocols, and ensure sufficient supplies are provided.
Link to article: https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(20)30460-8/fulltext
PDF:  The psychological impact of quarantine and how to reduce it: rapid review of the evidence
The psychological impact of quarantine and how to reduce it: rapid review of the evidence
CDC’s Crisis and Emergency Risk Communication (CERC) manual
COVID-19 is creating immense psychosocial disturbances. The CDC has produced a Crisis and Emergency Risk Communication (CERC) manual to instruct health responders and communicators on how to deal with the extraordinary mental and emotional stressors on people.
Link to Manual: https://emergency.cdc.gov/cerc/manual/index.asp
Covert coronavirus infections could be seeding new outbreaks
The data confirms that some infected people “can be highly contagious when they have mild or no symptoms. Urgent measures are needed to curb mild and asymptomatic cases that are fuelling the pandemic. This bolsters the case for closing schools, cancelling public gatherings and generally keeping people at home and out of public spaces.
Link to article: https://www.nature.com/articles/d41586-020-00822-x
Response to COVID-19 in Taiwan Big Data Analytics, New Technology, and Proactive Testing
Shows Taiwan as an example of how a society can respond quickly to a crisis and protect the interests of its citizens. Taiwan’s government learned from its 2003 SARS experience and established a public health response mechanism for enabling rapid actions for the next crisis. Well-trained and experienced teams of officials were quick to recognize the COVID-19 crisis and activated emergency management structures to address the emerging outbreak.
Link to article: https://jamanetwork.com/journals/jama/fullarticle/2762689
The Demand for Inpatient and ICU Beds for COVID-19 in the US: Lessons From Chinese Cities
In this pre-print researchers analyzed the timing of control measures and of community spread of COVID-19 in the Chinese cities of Wuhan and Guangzhou from January 10 to February 29, 2020. Early intervention resulted in Guangzhou having “lower epidemic sizes and peaks” than Wuhan in the first wave of the outbreak.
Link to paper: https://dash.harvard.edu/handle/1/42599304
Will the Coronavirus Ever Go Away? Here’s What One of the WHO’s Top Experts Thinks
Time magazine interviews Dr. Bruce Aylward, the senior adviser to the Director-General of the WHO, is one of the world’s top officials in charge of fighting the coronavirus pandemic. Dr. Aylward has almost 30 years of experience in fighting polio, Ebola and other diseases, and now he’s turned his attention to stopping the spread of COVID-19.
Link to article: https://time.com/5805368/will-coronavirus-go-away-world-health-organization/
Preparedness and vulnerability of African countries against importations of COVID-19: a modelling study
Evaluates the preparedness and vulnerability of African countries against their risk of importation of COVID-19.
Link to text: https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(20)30411-6/fulltext
Fact Check: Will Warm Weather Kill Coronavirus?
Fact checking: will warm weather kill the Coronavirus? More research needs to be done.
Link to article: https://www.snopes.com/fact-check/coronavirus-warm-weather/
Rapid Response was Crucial to Containing the 1918 Flu Pandemic
In the case of the 1918 flu pandemic, research has shown that the faster authorities moved to implement the kinds of social distancing measures designed to slow the transmission of disease, the more lives were saved.
Substantial undocumented infection facilitates the rapid dissemination of novel coronavirus (SARS-CoV2)
These findings explain the rapid geographic spread of SARS-CoV2 and indicate containment of this virus will be particularly challenging.
Link to article: https://science.sciencemag.org/content/early/2020/03/13/science.abb3221.full
SARS-CoV-2 is not a laboratory construct
New research “clearly show that SARS-CoV-2 is not a laboratory construct or a purposefully manipulated virus”
The proximal origin of SARS-CoV-2 https://www.nature.com/articles/s41591-020-0820-9
Coronavirus: The Hammer and the Dance
Not a peer-reviewed paper but we deem it useful and interesting. It explores how strong coronavirus measures today should only last a few weeks, there shouldn’t be a big peak of infections afterward, and it can all be done for a reasonable cost to society, saving millions of lives along the way.
Link to article: https://medium.com/@tomaspueyo/coronavirus-the-hammer-and-the-dance-be9337092b56
High Temperature and High Humidity Reduce the Transmission of COVID-19
Preliminary results of how air temperature and humidity influence the transmission of COVID-19.
PDF:  High Temperature and High Humidity Reduce the Transmission of COVID-19
High Temperature and High Humidity Reduce the Transmission of COVID-19
An interactive web-based dashboard to track COVID-19 in real time
Paper on an online interactive dashboard, hosted by the Center for Systems Science and Engineering (CSSE) at Johns Hopkins University, Baltimore, MD, USA, to visualise and track reported cases of coronavirus disease 2019 (COVID-19) in real-time.
Link to text: https://www.thelancet.com/journals/laninf/article/PIIS1473-3099(20)30120-1/fulltext
PDF:  An interactive web-based dashboard to track COVID-19 in real time
An interactive web-based dashboard to track COVID-19 in real time
Decoding evolution and transmissions of novel pneumonia coronavirus (SARS-CoV-2) using the whole genomic data
Phyloepidemiologic analyses indicated the SARS-CoV-2 source at the Hua Nan market should be imported from other places. The crowded market boosted SARS-CoV-2 rapid circulations in the market and spread it to the whole city in early December 2019.

